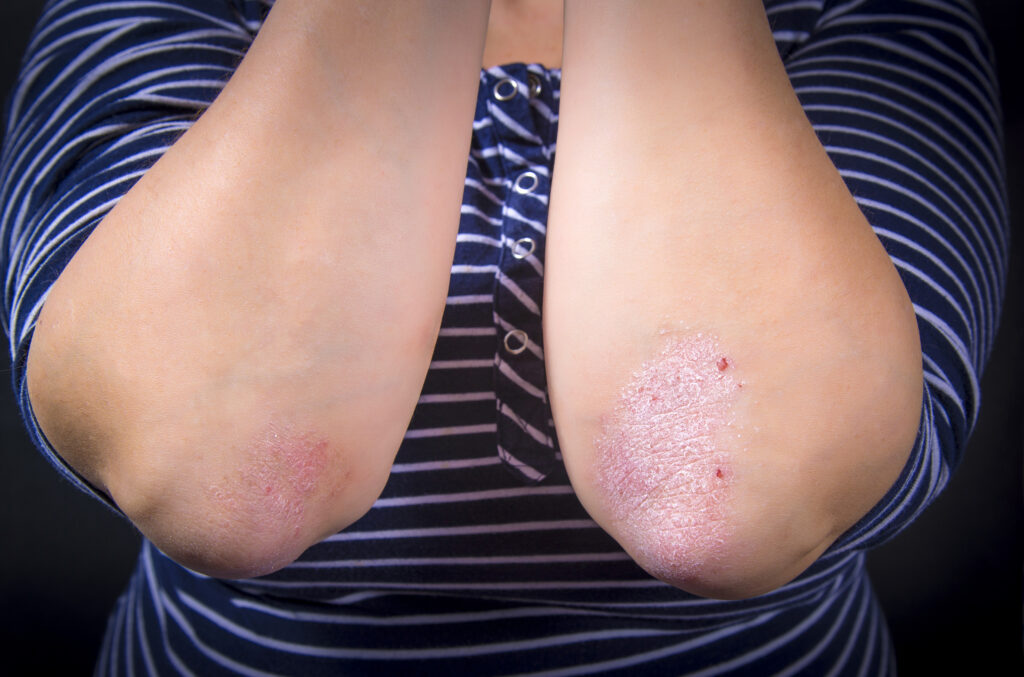
Psoriasis is just a minor irritation to the skin for some people, but it can have a significant impact on quality of life for those more severely affected.
Psoriasis is just a minor irritation to the skin for some people, but it can have a significant impact on quality of life for those more severely affected.
As psoriasis is unpredictable and chronic disease, it is necessary to understand the disease, its treatment and its effect on other body parts. If you are suffering from psoriasis you should get your doubts clarified from your doctor for proper management of the disease. You can ask following questions to your doctor:
1) What is psoriasis and what is the pathology behind it?
Psoriasis is a persistent, long-lasting (chronic), autoimmune disease which affects the skin and other body parts.
Our skin is mainly made up of two layers: epidermis (outer layer) and dermis (inner layer). The cells of the epidermis are originated in the dermis and then they move up towards the surface. At a regular interval of 28-30 days, the cells of the epidermis are replaced by new cells formed in the dermis.
In psoriasis, this process of cell production in the dermis is sped up. New cells are formed and moved upward to the skin surface faster than they can be incorporated into skin. The excess cells accumulate and are scaled off in the form of flakes.
In psoriasis, the skin becomes inflamed and red eruptions appear on the surface of the skin that begins to itch excessively. These areas form thickened areas (plaques) that are covered with silvery scales over the reddened lesions.
In spite of a range of options, effective treatment of psoriasis can be challenging.
Read more on the diagnosis of psoriasis.
2) What is the course of the disease?
There may be times when your psoriasis symptoms get better (remission) alternating with times with flare up (relapse). The disease is unpredictable, going through cycles of remission and relapse.
Psoriasis is categorized as mild, moderate, or severe, depending on the percentage of body surface involved and the impact on the patient’s quality of life.
[box type=”note” ]We treat patients from USA, UK, Canada, Australia, UAE & 180 more countries. Get an expert opinion on your ailment, click here to ask Dr. Shah’s team directly.[/box]
3) What are the triggering factors for relapse?
Conditions that may cause flares include infections, stress, and cold, dry weather seems to make psoriasis worse for many patients. Also, certain medicines, including beta-blockers, which are prescribed for high blood pressure, and lithium may trigger an outbreak or worsen the disease.
Sometimes people who have psoriasis notice that lesions will appear where the skin has experienced trauma (Conner’s phenomena). The trauma could be from a cut, scratch, sunburn, or infection.
4) Can psoriasis affect any part of my body? Is psoriasis is contagious?
Commonly affected areas are elbows, knees, other parts of the legs, scalp, lower back, face, palms, and soles of the feet, but they can occur on skin anywhere on the body.
The disease may also affect the fingernails, the toenails, and the soft tissues of the genitals, and inside the mouth.
Some people with psoriasis experience joint inflammation that produces symptoms of arthritis. This condition is called psoriatic arthritis.
Psoriasis is not contagious and cannot be transmitted from person to person.
5) What causes psoriasis? Is this a hereditary disease?
Psoriasis is an autoimmune disease, meaning that an individual’s immune system attacks its own tissues.
Risk factors may contribute to onset of disease:
Family history: A person with family history of psoriasis has higher chances of getting it.
Environmental factors : Certain things can trigger or worsen psoriasis in people who already have the disease or who are at increased risk of developing it. This include:
- Stress
- Injury to your skin
- Diet
- Smoking, Alcohol
- Certain types of medications
Read about the causes of psoriasis.
6) What is an autoimmune disease?
The immune system protects the body from infections by identifying ‘foreign entities’ such as viruses and bacteria and removing them.
Individuals with an autoimmune disease have an immune system that fails to recognize ‘self’ from ‘non-self’ resulting in an immune response against the perceived ‘foreign entity’ and inflammation.
7) Can psoriasis be cured? What are the available treatment options?
Psoriasis is a difficult disease to treat. It has been a challenge to the medical faculty, as most cases of psoriasis tend to relapse after using any kind of currently available treatments. Psoriasis can be controlled effectively with the proper treatment.
Doctors generally treat psoriasis in steps based on the severity of the disease, type of psoriasis, areas affected and the patient’s response to initial treatments.
[box type=”note” ]Get expert opinion from our doctors. Just send your query here.[/box]
Conventional Treatment :
The conventional medicines or so-called allopathic or modern medicine uses more of the following medicines, all of them are immunosuppressive medicine in some way or the other.
- Psoralen (with or without P-UV rays) (Oral)
- Cortisone (Oral, injections, topical)
- Methotrexate (Oral)
- Cyclosporine (Oral)
- Retinoids (Oral)
Ayurvedic and Herbal treatment:
Certain herbs and Ayurvedic medicines have been found to effective for the treatment of psoriasis. The treatment entails the use of plants, salts, churnas, chemicals (Rasayana) in different forms, along with yoga, pranayama, body cleansing, and correcting food habits.
Homeopathic treatment:
It aims at addressing the immunological factors responsible for its development. The immune system is governed by a host of factors such as genetic, environmental, physical, emotional, hormonal factors, etc. So, homeopathy aims considering the totality of the person who has psoriasis.
8) What type of medicines are you prescribing for me, and how does it work? What are the side effects of treatment?
If your doctor is treating you with conventional medicines, you should ask about the side effects of the medicines prescribed. Immunosuppressive medicines lower immunity and affect other body parts as well.
Whereas homeopathic treatment is free from any side effects. Homeopathic medicines. It stimulates body’s own healing process and works at the root level to restore the deviated immunity back to normalcy.
Know more about homeopathy treatment for Psoriasis.
9) How much Time does it take to treat psoriasis?Do I need to take the treatment lifelong?
Psoriasis is an obstinate and chronic disease. The disease is unpredictable, going through cycles of remission and relapse but with a proper treatment frequency of the relapse can be reduced and long remission period can be achieved.
There is no shortcut to its cure. The length of treatment varies from case to case, depending on the duration of Psoriasis, areas affected, the extent of spread, previous medication , general health and associated diseases etc.
If psoriasis is treated using immunosuppressive medicines such as cortisone or Methotrexate, there is a possibility that it resurfaces with more intensity and may turn more difficult in treating. If Psoriasis is treated with homeopathy in the early phase, the overall control of the disease in future is much better.
Know about the adverse effects of Methotrexate here.
Read the homeopathy remedies to treat psoriasis.
10) What other lifestyle changes will help me in proper management of my disease?
Stressful life events seem to make psoriasis worse in many people. Try to avoid stress as much as possible. Exercise is beneficial for psoriasis because it relieves stress. If you exercise outdoors, your skin may also benefit from the exposure to ultraviolet light.
Eliminating animal proteins in the form of red meat helps. Fatty food, dairy products, and processed food, artificially flavored food, if eliminated, can help symptomatically. Omega 3s rich food such as flaxseeds, olive oil, pumpkin seeds and walnuts are useful to control the disease process.
After getting answers for above questions regarding psoriasis I am sure you would like to go for a treatment which is safe, gentle and long lasting. Homeopathy should be your first option in that case . Get in touch with us to know how Dr. Rajesh Shah’s research based homeopathy treatment for psoriasis at LifeForce can help you. You can give us a call at +91-22-66888888 or drop in an email at info@lifeforce.in
Before-after photographs of patients suffering from psoriasis treated successfully at Life Force.
[box type=”note” ]Got Questions? Get answers to all the questions regarding your ailment from Dr. Shah directly.[/box]
– Written by Dr. Aparna Hingmire Associate Doctor to Dr. Rajesh Shah, Team LifeForce.